The 2026 medicare advantage outlook
Medicare Advantage (MA) plans have become increasingly popular, covering over 50% of all Medicare beneficiaries as of 2023. These plans, offered by private insurance companies, bundle Part A, Part B, and often Part D benefits, and frequently include extras like vision, dental, and hearing care. For 2026, the Centers for Medicare & Medicaid Services (CMS) is introducing several updates that will impact what MA plans cover, and how much they cost.
The 2026 updates aren't a total rewrite, but they change the math for anyone on a fixed income. Premiums are shifting and there is a clear move toward covering more preventative care. It looks like a push for comprehensive coverage, though that rarely means things get simpler or cheaper for the person paying the bill.
According to CMS data released in November 2023, the average monthly premium for MA plans is expected to remain relatively stable in 2026. However, this average masks a lot of variation. Some plans are seeing premium increases, while others are actually decreasing. The real story is in the benefits within those plans. This is where the changes regarding technology and healthcare devices come into play.
Those already enrolled in an MA plan should expect to receive an Annual Notice of Change (ANC) in the fall of 2025, detailing any changes to their coverage. If you're new to Medicare or considering switching plans, now is the time to start researching your options. It's a complex system, and understanding these changes is the first step to making an informed decision.
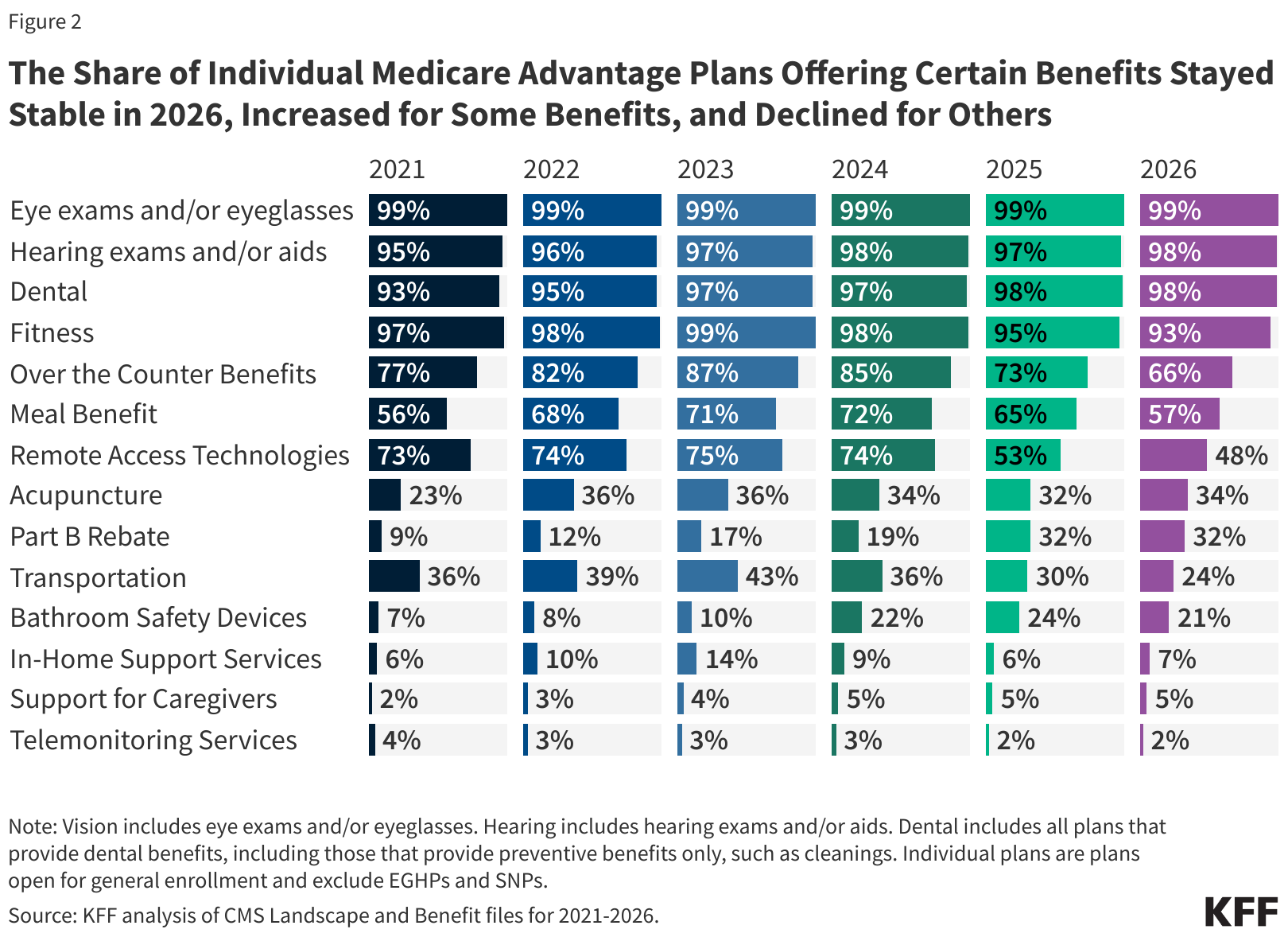
New Coverage Areas: What's Changing?
The CMS updates for 2026 are focused on expanding access to preventative care and chronic disease management. A key component of this is increased flexibility for MA plans to offer benefits beyond what’s traditionally covered by Original Medicare. This includes things like home-based medical services, transportation to healthcare appointments, and – crucially for our focus – expanded coverage for remote patient monitoring (RPM) and telehealth.
Specifically, CMS is encouraging plans to offer more comprehensive supplemental benefits for individuals with chronic conditions. This could translate to broader coverage for devices used to manage conditions like diabetes, heart disease, and respiratory illnesses. However, it's important to note that plans aren't required to offer these benefits; it's up to each individual plan to decide what to include. The 2026 Medicare and You Handbook details these options.
One area with potential changes is the intersection of the Inflation Reduction Act (IRA) and MA benefits. The IRA caps out-of-pocket prescription drug costs for those in Medicare, and the way these savings interact with MA plans is still being clarified. It's possible that some plans will adjust their drug coverage in response to the IRA, potentially leading to changes in premiums or formularies. This is something to watch closely.
Currently, many MA plans offer some level of coverage for telehealth services, but the extent of that coverage varies significantly. The 2026 changes aim to standardize and expand access to telehealth, particularly for behavioral health services. We’re likely to see more plans covering virtual mental healthcare sessions and online therapy platforms.
- Increased flexibility for MA plans to offer supplemental benefits.
- Focus on preventative care and chronic disease management.
- Potential adjustments to drug coverage due to the Inflation Reduction Act.
- Expanded access to telehealth, especially behavioral health services.
Medicare Advantage Coverage: 2024/2025 vs. Projected 2026
| Device/Service | Current Coverage (2024/2025) | Projected Coverage (2026) | Key Changes | Potential Out-of-Pocket Costs |
|---|---|---|---|---|
| Hearing Aids | Coverage varies significantly by plan. Some plans offer limited hearing aid benefits, often as an extra benefit. Many plans do *not* cover routine hearing care. | The CMS is encouraging plans to expand benefits, but coverage is still expected to vary. Increased focus on preventative care may include hearing screenings. | Potential for more plans to include some hearing aid coverage, but likely with limitations on brands or models. Increased emphasis on hearing wellness programs. | Varies widely; can range from several hundred to several thousand dollars depending on the aid and plan. Copays for screenings may apply. |
| Vision Care | Many Medicare Advantage plans include vision coverage, typically covering eye exams and prescription glasses or contacts. Coverage levels differ considerably. | Continued availability of vision benefits is expected, with potential for increased coverage of routine vision services. Some plans may expand coverage to include enhanced lens options. | Expect continued variation in plan benefits, with some plans offering more comprehensive vision care than others. Focus on preventative eye health. | Copays for exams ($20-$50) and allowances for glasses/contacts ($100-$300) are common. Higher-end options typically require additional out-of-pocket expense. |
| Dental Care | Dental coverage is a common extra benefit in Medicare Advantage plans, but it’s rarely comprehensive. Often includes preventative services (cleanings, exams) and some coverage for basic restorative care. | Dental coverage is expected to remain a popular extra benefit. Plans may continue to offer varying levels of coverage, with a focus on preventative services. | Continued variation in coverage levels. Plans may offer different tiers of dental benefits with varying premiums. | Copays for preventative care ($20-$50) are common. Restorative care (fillings, extractions) typically has higher out-of-pocket costs or a limited annual maximum. |
| Remote Patient Monitoring (RPM) Devices | Increasingly covered by Medicare Advantage, particularly for chronic conditions like diabetes and heart failure. Coverage often includes the device and monitoring services. | The CMS continues to support the expansion of RPM. Expect broader coverage for a wider range of conditions and potentially more advanced devices. | Expansion of covered conditions and device types. Increased focus on data integration and remote care coordination. | May require a copay for the device or monitoring services. Costs vary depending on the condition and device. |
| Wearable Fitness Trackers (for Health Programs) | Generally *not* covered as a standard benefit, although some plans may offer discounts or reimbursements as part of wellness programs. | Coverage remains unlikely as a standard benefit. However, some plans may integrate wearable data into wellness programs and offer incentives for participation. | Potential for increased integration with wellness programs, but direct coverage is not expected. | Costs are typically borne by the individual, though some plans may offer discounts or reimbursements. |
| Digital Health Tools (Apps for Medication Management) | Coverage is limited. Some plans may offer access to digital health tools as part of wellness programs, but they are not typically covered as a medical expense. | Similar to fitness trackers, direct coverage is unlikely. Plans may partner with digital health companies to offer access to apps and tools. | Continued reliance on wellness programs and partnerships rather than direct coverage. | Costs are generally borne by the individual, though some plans may offer free or discounted access. |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
How remote monitoring actually works
Remote Patient Monitoring (RPM) is where technology really starts to shine in healthcare. It involves using devices – like blood pressure cuffs, glucose meters, and pulse oximeters – to collect health data outside of a traditional clinical setting. This data is then transmitted to healthcare providers, allowing them to monitor a patient’s condition remotely. It's a big shift from relying solely on in-person appointments.
What devices qualify for RPM coverage? Generally, it includes devices used to track vital signs, weight, and activity levels. The data must be electronically transmitted to the provider for it to be considered RPM. Conditions typically monitored through RPM include diabetes, hypertension, heart failure, and chronic obstructive pulmonary disease (COPD). The specific conditions covered will vary by plan, of course.
The benefits of RPM are clear: early detection of health issues, reduced hospital readmissions, and improved chronic disease management. For seniors, this can mean maintaining independence and avoiding unnecessary trips to the doctor’s office. However, there are challenges. Reliable internet access is essential, and many seniors may need assistance setting up and using the devices. Technical support is key.
Privacy and data security are also major concerns. Any RPM program must comply with HIPAA regulations to protect patient information. It’s important to understand how your data is being collected, stored, and used. You should also ask your provider about their data security protocols. I’ve seen some plans offer training sessions to help patients feel comfortable with the technology and address privacy concerns.
- Blood pressure cuffs, glucose meters, and pulse oximeters
- Commonly Monitored Conditions: Diabetes, hypertension, heart failure, COPD.
- Benefits: Early detection, reduced readmissions, improved chronic disease management.
- Challenges: Internet access, technical support, data privacy.
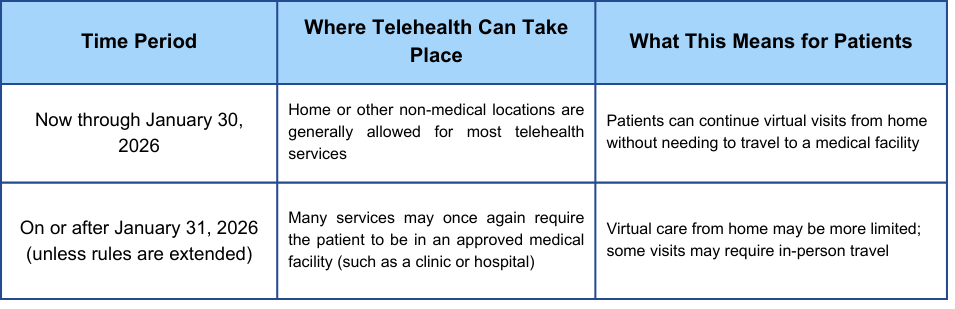
Telehealth Expansion and Virtual Care
Telehealth experienced a massive surge in popularity during the pandemic, and it’s here to stay. It allows patients to consult with healthcare providers remotely using video conferencing, phone calls, or secure messaging. The 2026 changes to Medicare Advantage are designed to further expand access to these virtual care options.
What’s changing specifically? We’re likely to see more MA plans covering a wider range of telehealth services, including specialist consultations, mental healthcare, and even physical therapy. CMS is also encouraging plans to offer virtual primary care, where patients can establish a relationship with a primary care physician who provides care entirely online. It’s a significant shift in how healthcare is delivered.
For seniors, telehealth offers several advantages: convenience, reduced travel time, and increased access to care, particularly for those living in rural areas or with mobility limitations. However, there are potential drawbacks. Some seniors may struggle with the technology, and the lack of a physical examination can be a concern for certain conditions. It’s not a perfect replacement for in-person care, but it can be a valuable supplement.
Virtual mental healthcare is a particularly important area of expansion. Many seniors face barriers to accessing mental health services, such as stigma and transportation difficulties. Telehealth can help overcome these barriers by providing convenient and confidential access to therapists and counselors. It’s a positive step towards addressing the growing mental health needs of the senior population.
- Benefits of Telehealth: Convenience, reduced travel, increased access.
- Potential Drawbacks: Technology challenges, lack of physical exam.
- Expanded Services: Specialist consultations, mental healthcare, virtual primary care.
Impact on Specific Devices: Hearing, Vision, and More
Let’s get down to specifics. How will these changes affect coverage for the devices seniors use most often? Hearing aids remain a tricky area. While Original Medicare doesn’t cover hearing aids, many MA plans do offer some level of coverage, often with limitations on the amount or type of aid covered. The 2026 changes may encourage plans to expand hearing aid benefits, but it’s not guaranteed.
Vision care is another area where MA plans often go beyond Original Medicare. Coverage for eyeglasses, contact lenses, and routine eye exams varies widely. Again, the 2026 updates could lead to more comprehensive vision benefits, but it’s up to each plan to decide. Dental care is also frequently included in MA plans, with coverage for preventative services, fillings, and dentures.
Mobility aids – walkers, wheelchairs, scooters – are generally covered by Original Medicare if deemed medically necessary. MA plans typically follow these guidelines, but they may have additional requirements or limitations. Durable medical equipment (DME), such as hospital beds and oxygen concentrators, is also covered under Medicare, and MA plans generally mirror this coverage.
When evaluating MA plans, pay close attention to cost-sharing requirements – deductibles, copays, and coinsurance – for these devices. Also, check if prior authorization is required, as this can add an extra step to the process. Don’t be afraid to call the plan directly and ask specific questions about their coverage policies. The 2026 Medicare and You handbook is a good place to start, but it’s not always comprehensive.
- Hearing Aids: Coverage varies widely; potential for expansion in 2026.
- Vision Care: Coverage for eyeglasses, contacts, and exams varies.
- Dental Care: Often included in MA plans.
- Mobility Aids & DME: Generally covered if medically necessary.
Resources for Senior Care
- Medicare.gov - The official U.S. government site for Medicare information. It offers a plan finder tool to compare Medicare Advantage plans and understand coverage details, including potential benefits for hearing, vision, and dental.
- Hearing Aid Centers of America - A network of audiologists offering a range of hearing aid options. Many accept Medicare Advantage plans, and some offer financing options to make hearing aids more affordable.
- Vision Source - A national provider of optometric care. They accept many Medicare Advantage plans and offer comprehensive eye exams, glasses, and contact lens fittings.
- Aspen Dental - A large branded dental services provider with locations across the US. They frequently work with Medicare Advantage plans for covered dental services like cleanings, fillings, and dentures.
- UnitedHealthcare Dental - Offers stand-alone dental plans and often includes dental benefits within their Medicare Advantage offerings. Check plan details for coverage levels and provider networks.
- Humana Dental - Similar to UnitedHealthcare, Humana provides both stand-alone dental plans and integrates dental coverage into many of its Medicare Advantage plans. Review specific plan benefits.
- AARP Dental Insurance Program (through Delta Dental) - While not directly Medicare, AARP members can access dental insurance plans through Delta Dental, which can supplement Medicare Advantage dental coverage.
Choosing the Right Medicare Advantage Plan
With these changes on the horizon, choosing the right Medicare Advantage plan is more critical than ever. Don’t just focus on the premium; consider the overall value of the plan, including its coverage for the technology and devices you need. Start by making a list of your healthcare priorities and any specific devices you use or anticipate needing.
When comparing plans, ask these questions: Does the plan cover the devices I use? What are the cost-sharing requirements? Is prior authorization required? Is my doctor in the plan’s network? What supplemental benefits are offered? Don’t assume that all plans are created equal; take the time to carefully review the plan details. I recommend using the Medicare Plan Finder tool on Medicare.gov.
It’s also important to understand the plan’s formulary – the list of covered drugs. If you take prescription medications, make sure your drugs are covered and that the cost is manageable. And remember, coverage can change from year to year, so it’s essential to review your plan annually during the Open Enrollment period (October 15 – December 7).
Don’t be afraid to seek help from a trusted source. State Health Insurance Assistance Programs (SHIPs) offer free counseling and assistance to seniors with Medicare questions. These programs can help you navigate the complex world of Medicare and choose a plan that meets your needs.
- Prioritize Your Needs: List your healthcare priorities and devices.
- Compare Plans Carefully: Review coverage, cost-sharing, and networks.
- Check the Formulary: Ensure your drugs are covered.
- Seek Assistance: Contact SHIPs for free counseling.
Have you ever had a Medicare claim denied?
Vote below to share your experience with Medicare claims and help us understand how coverage changes may affect seniors seeking healthcare devices and technology benefits.




No comments yet. Be the first to share your thoughts!