Medicare advantage and the 2026 telehealth shift
Big changes are coming to Medicare Advantage plans in 2026, and they center around telehealth. The Centers for Medicare & Medicaid Services (CMS) is expanding the types of telehealth services covered, aiming to make healthcare more accessible, especially for those in rural areas or with limited mobility. This isn’t just about having doctor’s appointments over video anymore; it's about a broader range of remote care options.
The 2026 expansion focuses on remote patient monitoring. You'll use home devices to track vitals and send that data to your doctor. CMS wants to catch health issues before they require a hospital stay, though the specific coverage rules depend entirely on which private insurer runs your plan.
For many older adults, navigating these changes can be daunting. Seniors Bot is here to help break down the new rules and explain how they impact coverage for senior healthcare devices. These updates are a significant step toward integrating technology into healthcare, but understanding the details is key to maximizing the benefits. It's a move toward preventative care, allowing doctors to intervene earlier when problems arise.
While these changes are largely positive, it’s important to remember that the specifics will depend on your individual Medicare Advantage plan. Don’t assume a service covered under original Medicare is automatically covered under your Advantage plan. We’ll explore the details and provide resources to help you understand your options.
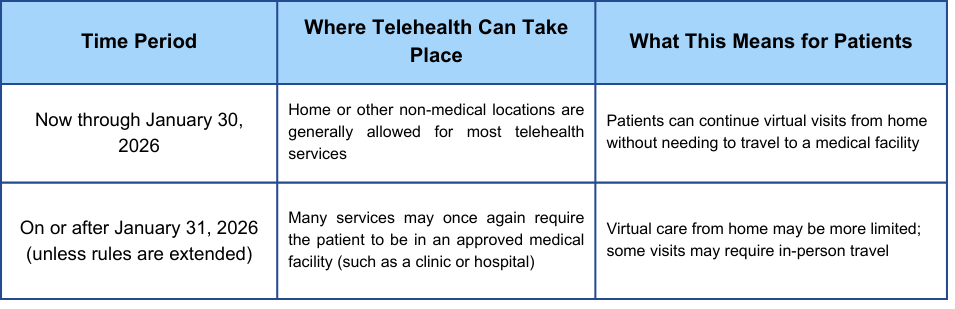
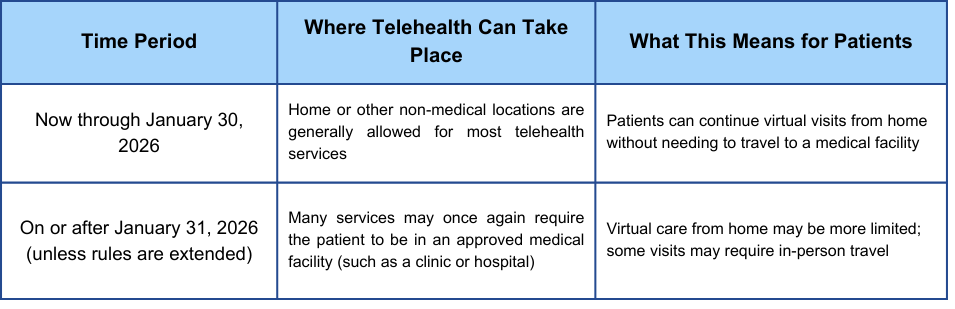
Remote patient monitoring expansion
Remote Patient Monitoring (RPM) is a key component of the 2026 Medicare Advantage changes. This involves using digital devices to collect health data outside of a traditional clinical setting. Think blood pressure cuffs, digital scales, and pulse oximeters – devices that allow your doctor to track your health between appointments. The data is then securely transmitted to your healthcare provider for review.
Conditions commonly monitored through RPM include heart failure, chronic obstructive pulmonary disease (COPD), diabetes, and hypertension. The goal is to identify potential problems early on and adjust treatment plans accordingly. This proactive approach can help prevent hospitalizations and improve overall health management. RPM isn’t a one-size-fits-all solution; it’s most effective when tailored to an individual’s specific needs.
The data from these devices is typically transmitted wirelessly – often via Bluetooth or cellular connection – to a secure platform accessible by your doctor. Your healthcare team will then analyze the data and reach out if any concerning trends are detected. It’s important to understand that RPM isn’t meant to replace regular doctor visits, but rather to supplement them. It provides a more continuous picture of your health.
According to CMS guidelines, documentation is essential for RPM reimbursement. Providers must demonstrate the medical necessity of the monitoring and provide detailed records of data transmission and review. This falls under the Durable Medical Equipment (DME) requirements, as outlined in CMS publication A55426. Proper documentation ensures claims are processed correctly and patients receive the care they need.
- Common RPM devices include blood pressure monitors, scales, and pulse oximeters.
- Conditions Monitored: Heart failure, COPD, diabetes, hypertension
- Data Transmission: Wireless via Bluetooth or cellular connection
- Documentation: Essential for reimbursement; follows DME guidelines (CMS A55426)
Which devices are covered?
Determining exactly which senior healthcare devices Medicare Advantage will cover is complex. Coverage varies significantly between plans, so it’s vital to check your specific plan details. However, we can outline categories of devices that may be eligible for coverage under the expanded telehealth benefits. Remember, 'may' is the operative word here.
For cardiovascular health, blood pressure monitors are often covered, especially for those with hypertension. Smart scales fall into the weight management category and could be eligible for coverage if your doctor deems weight management medically necessary. Pulse oximeters, used to measure blood oxygen levels, are frequently covered for individuals with respiratory conditions like COPD.
Fall detection devices are gaining attention, but coverage is less certain. While incredibly useful, they’re often viewed as convenience items rather than medical necessities. Some plans might offer a partial reimbursement or a discount on these devices. Coverage for mental health-related devices, like those used for remote therapy, is also emerging, but still varies widely.
Important Disclaimer: Coverage is not guaranteed. Always verify with your specific Medicare Advantage plan to confirm whether a particular device or service is covered. Look for the Evidence of Coverage document, or call your plan’s member services line. Don't rely on general information; get the details specific to your plan.
Telehealth Beyond Video: New Service Types
The expansion of telehealth isn't limited to virtual doctor's appointments. Medicare Advantage plans are now covering a wider range of services delivered remotely. This includes remote physical therapy, allowing patients to receive rehabilitation exercises and guidance from a therapist in the comfort of their own homes. It’s a convenient option for those with mobility issues or transportation challenges.
Mental health counseling is also seeing a surge in telehealth availability. Remote therapy sessions can be particularly beneficial for seniors who may feel uncomfortable seeking in-person care or who live in areas with limited access to mental health professionals. Chronic disease management programs, delivered through telehealth platforms, are another growing trend. These programs often involve regular check-ins with a health coach and personalized support to help patients manage their conditions.
Compared to traditional in-person care, telehealth offers increased convenience and accessibility. However, it’s not without drawbacks. Some seniors may prefer the personal connection of in-person visits, and technology barriers can be a challenge. It’s also essential to consider privacy and security concerns when using telehealth services. Ensure the platform is HIPAA compliant and that your personal health information is protected.
These new service types offer a more holistic approach to healthcare, addressing not only physical health but also mental and emotional well-being. The key is finding a balance between telehealth and traditional care that meets your individual needs and preferences.
Fall Detection Tech: A Closer Look
Fall detection technology is becoming increasingly popular among seniors and their families. These devices aim to provide peace of mind by automatically alerting emergency services if a fall is detected. They come in two main forms: wearable devices and ambient sensors. Wearable devices, like smartwatches and pendants, use accelerometers to detect sudden changes in motion indicative of a fall.
Ambient sensors, on the other hand, are placed around the home and use cameras or other technologies to monitor movement patterns. Accuracy rates vary depending on the device and the environment. Wearable devices generally have higher accuracy rates, but require the user to wear the device consistently. The MIT News article details an eldercare robot designed to assist with sitting, standing, and preventing falls—a more proactive approach.
When a fall is detected, the device typically attempts to contact the user first. If there's no response, it automatically alerts emergency services and designated contacts. However, false alarms can occur, so it’s important to understand the device’s sensitivity settings and how to minimize false positives. The cost of fall detection devices ranges from around $50 for a basic pendant to several hundred dollars for a more advanced smartwatch or sensor system.
Medicare Advantage coverage for fall detection devices is often limited. Because these are often considered safety devices rather than medical necessities, plans are less likely to cover the full cost. Some plans might offer a partial reimbursement or a discount, but it’s not guaranteed. It’s crucial to check your plan’s specific coverage policies before purchasing a device.
Navigating Plan Options & Enrollment
Choosing a Medicare Advantage plan that meets your telehealth needs requires careful research. Start by visiting the official Medicare website () to compare plans available in your area. Pay close attention to the plan’s coverage for telehealth services and devices, as well as the cost-sharing requirements (copays, deductibles, etc.).
When comparing plans, ask these key questions: Does the plan cover remote patient monitoring? What types of telehealth services are included? Are there any restrictions on which providers you can see via telehealth? What is the cost of covered devices? Don’t hesitate to call the plan directly to get clarification on any unclear policies.
Enrollment in Medicare Advantage typically occurs during the Annual Enrollment Period (October 15 – December 7). There are also Special Enrollment Periods available if you qualify. Missing the enrollment deadline could mean you have to wait until the next enrollment period to make changes to your coverage. Be mindful of these deadlines to avoid gaps in your healthcare coverage.
State Health Insurance Assistance Programs (SHIPs) offer free, unbiased counseling to help seniors navigate Medicare. SHIP counselors can assist you with comparing plans, understanding your benefits, and enrolling in coverage. You can find your local SHIP office by visiting the Medicare website or calling 1-800-MEDICARE.




No comments yet. Be the first to share your thoughts!