Telehealth expansion in Medicare Advantage
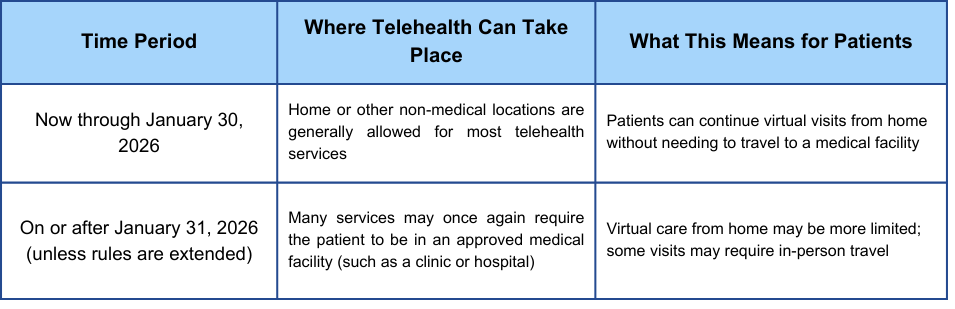
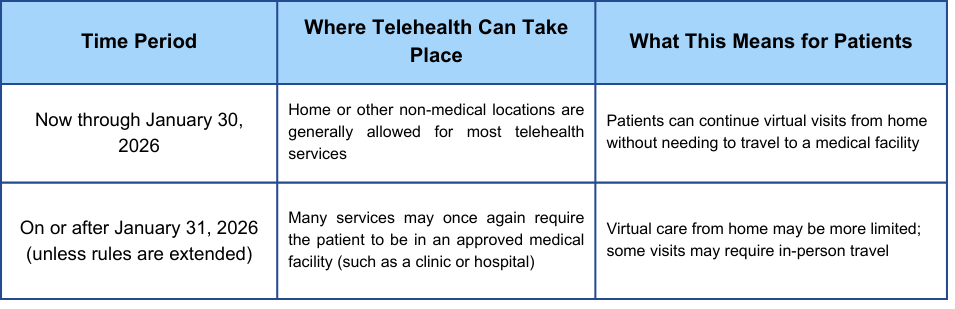
For 2026, Medicare Advantage plans are set to undergo significant changes regarding telehealth coverage. These aren’t just tweaks around the edges; the Centers for Medicare & Medicaid Services (CMS) is pushing for greater flexibility in how these plans deliver remote care. This means potentially more services offered virtually, and a wider range of senior healthcare devices supported by your insurance.
CMS is moving toward more accessible care for seniors with mobility issues or those in rural areas. Previously, Medicare Advantage plans often required you to have a pre-existing relationship with a provider before they would pay for a video visit. The 2026 guidelines remove many of those restrictions.
What's different is the emphasis on preventative care and continuous monitoring. We’re moving beyond simply replacing an in-person doctor's visit with a video call. The focus is now on using technology to proactively manage health and prevent emergencies. This change will likely influence which senior healthcare devices are considered medically necessary and therefore covered by your plan.
Which remote monitoring devices are covered?
The expansion of telehealth coverage naturally leads to the question: what remote patient monitoring (RPM) devices will Medicare Advantage plans cover? While specifics vary from plan to plan, several categories are likely to see increased coverage. These include devices for tracking vital signs, such as blood pressure cuffs, glucose monitors, and pulse oximeters.
Fall detection sensors are also a key area of interest, which we'll cover in more detail later. Beyond these, plans may also cover devices for monitoring weight, activity levels, and even sleep patterns. The goal is to provide a more complete picture of a senior’s health status outside of traditional clinical settings.
Coverage isn't automatic. CMS documentation (A55426) shows that these devices usually fall under Durable Medical Equipment (DME). To get a claim approved, you need a doctor’s order stating the device is medically necessary, a plan for how your data is used, and proof you’ve been trained to use the hardware.
Don’t assume a device is covered simply because it’s telehealth-related. It’s crucial to check your plan’s formulary – the list of covered drugs and devices – and understand any cost-sharing requirements, such as copays or deductibles. Calling your plan directly is the best way to get a definitive answer.
Remote Patient Monitoring (RPM) Devices & Potential Medicare Advantage Coverage - 2026 Outlook
| Device Type | Typical Senior Use Case | Coverage Likelihood (Based on Current Trends) | Notes |
|---|---|---|---|
| Blood Pressure Monitor | Managing hypertension, detecting potential cardiovascular issues. | High | Increasingly covered as part of chronic condition management programs. Many plans already include basic coverage. |
| Pulse Oximeter | Monitoring blood oxygen levels, particularly for seniors with COPD or heart failure. | Medium | Coverage often tied to specific diagnoses and demonstrated need. Telehealth expansion may broaden access. |
| Digital Weight Scale | Tracking weight changes, important for heart failure and edema management. | Medium | Frequently included when bundled with other RPM services, focusing on fluid management. |
| Glucose Meter | Managing diabetes, tracking blood sugar levels. | High | A standard offering in many Medicare Advantage plans with diabetes management programs. |
| Activity Tracker (with heart rate monitoring) | Monitoring activity levels, sleep patterns, and heart rate; fall detection capabilities. | Medium | Coverage is growing, especially for fall risk reduction programs, but often requires a prescription and plan approval. |
| Connected Thermometer | Remote temperature monitoring, useful for detecting early signs of infection. | Low to Medium | Coverage is less common as a standalone device, but may be included in broader telehealth packages focusing on infection control. |
| Medication Adherence Monitor | Tracking medication intake to improve compliance. | Low | Coverage is currently limited, but may increase with a greater focus on medication management within telehealth. |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Fall detection tech and Medicare Advantage
Fall detection devices are gaining popularity among seniors and their families, and the new telehealth rules could potentially increase coverage for these life-saving technologies. These devices come in two main forms: wearable devices like smartwatches or pendants, and ambient sensors that can be placed around the home.
Wearable devices typically use accelerometers to detect sudden falls and can automatically alert emergency services or designated contacts. Ambient sensors, on the other hand, use cameras or other technologies to monitor movement patterns and identify potential falls. The integration of these devices with emergency response services is a major benefit.
Coverage for fall detection is still hit-or-miss. While the new rules allow plans to cover them, many insurers still label these as 'convenience' items rather than medical necessities. You'll have to check your specific plan. If you call your provider, explain how the device prevents hospitalizations—that's the language they respond to.
- Step 1: Check your plan’s formulary for fall detection devices.
- Step 2: Contact your plan’s customer service to inquire about coverage.
- Step 3: Ask about any specific requirements for documentation or prior authorization.
Managing chronic conditions
Expanded telehealth coverage has the potential to significantly improve the management of chronic conditions common in seniors, such as heart disease, diabetes, and COPD. Remote patient monitoring devices allow healthcare providers to track key health indicators – like blood pressure, blood sugar levels, and oxygen saturation – on an ongoing basis.
This continuous stream of data provides a more complete picture of a patient’s condition than sporadic in-person visits alone. Providers can use this information to identify potential problems early on and adjust treatment plans accordingly. For example, a sudden spike in blood pressure could trigger a virtual consultation with a doctor, preventing a potentially serious health event.
The benefit isn’t just about reacting to problems; it’s about proactive care. RPM devices can empower seniors to take a more active role in their own health management. By tracking their own data and sharing it with their healthcare team, they can gain a better understanding of their condition and make informed decisions about their lifestyle. This isn’t simply about convenience, but about the potential for better health outcomes.
How to choose a plan
Choosing the right Medicare Advantage plan can be overwhelming, especially with the new telehealth benefits to consider. Start by carefully reviewing each plan’s formulary to see which remote patient monitoring devices are covered. Pay attention to any cost-sharing requirements, such as copays, deductibles, and coinsurance.
Next, check the plan’s provider network to ensure that your preferred doctors and hospitals are included. Also, consider the plan’s star rating – a measure of its quality and performance. Plans with higher star ratings generally offer better benefits and customer service.
Don't hesitate to call the plan directly and ask specific questions about telehealth coverage. Ask about the documentation requirements for DME claims, the process for getting a device approved, and any limitations on the types of services that are available remotely. Reading the fine print is essential, and don’t be afraid to ask for clarification if something is unclear.
- Review the plan’s formulary to see which specific monitors are listed.
- Check the provider network.
- Consider the plan’s star rating.
- Call the plan with specific questions.

Data privacy and security
The increased reliance on telehealth and remote patient monitoring devices raises legitimate concerns about data privacy and security. These devices collect sensitive personal health information, which could be vulnerable to cyberattacks or unauthorized access. It’s crucial to understand the risks and take steps to protect your data.
Ensure that your healthcare providers and insurance plans are HIPAA compliant – meaning they adhere to federal standards for protecting patient privacy. Ask about the security measures they have in place to safeguard your data, such as encryption and access controls. Be wary of sharing your personal health information with unverified sources.
When using telehealth platforms, make sure the connection is secure. Look for the “https” in the web address and a padlock icon in your browser. Use strong passwords and enable two-factor authentication whenever possible. While the benefits of telehealth are significant, it’s important to be vigilant about protecting your privacy.




No comments yet. Be the first to share your thoughts!